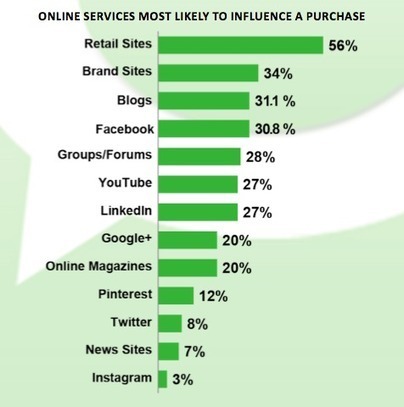
Here they are:
Patients want doctors to treat them as partners. Patients expect their doctors to listen to them not only about their symptoms, but also about their own perspectives on their condition. To be clear, patients don’t want to play doctor, but many patients—especially those with rare diseases—become highly educated about their condition and have done research which they believe bears consideration. The asymmetry of medical information available to patients versus doctors is almost gone, and today any one of us can go online to learn a great deal about a medical condition.
Patients are less cynical about pharma companies than you’d think. Patients want the medical system to work for them. They want pharma companies to make the drugs that help them and their loved ones. When we started Inspire, we were warned that patients would be overwhelmingly negative about pharma companies. This is simply not what we see. What we do see is a lot of discussion about how to optimize treatment, and a genuine interest among patients to best to benefit from their treatments.
Patients are not online just to vent. In our experience, patients seek three kinds of support: emotional, scientific, and practical. Many patients get scientific support from their physicians and online encyclopedic sources. But they are also hungry for practical information to improve their health, and they gather a lot of this information from their peers online. In two recent Inspire surveys—one of psoriasis patients, and another patients with the rare disease neurofibromatosis—each group said the primary reason they participated in online groups was to research the best available treatments. Emotional support and empathy are important, no doubt. But many patients share crucial practical information that only fellow patients know.
Patient communities aren’t ‘soft.’ The notion that patient-provided information is less important or valuable than physician-provided information is wrong. Different? Yes. Inferior? No. One only needs to spend ten minutes in our ovarian cancer group, for example, to immediately realize there is a great deal of knowledge and benefit being shared among patients 24 hours a day. This is in no way less rigorous or serious than traditionally authoritative sources of information. What is clear to us is this: patients who want to educate themselves about their health seek multiple sources of information, and they are smart enough to weigh those sources appropriately. To suggest patient-to-patient information about treatment options and decision-making is not as good as other kinds of support is patronizing and simply wrong.
Patients are generous. Patients, even some who are gravely ill, give of themselves in online groups in profound ways. It is clear to us that patients want to help one another, and in doing so, many discover they help themselves.

 Recently,
Recently,